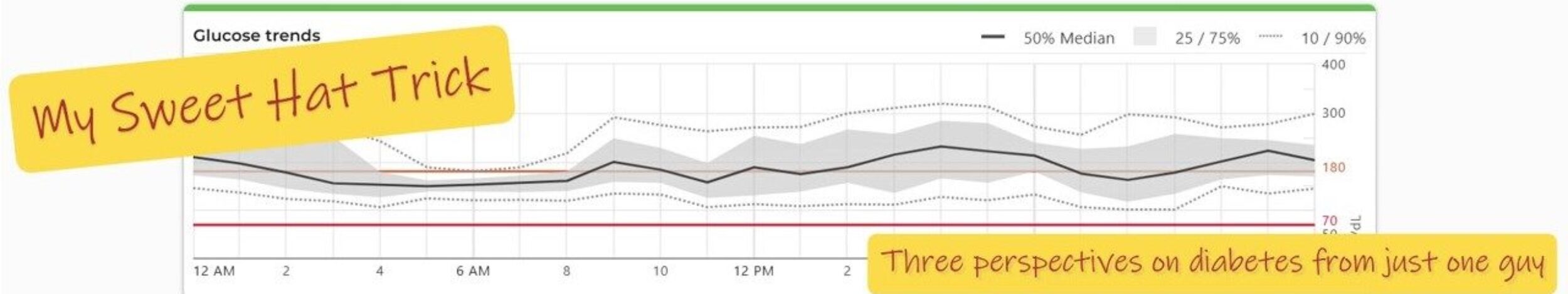
“I know my A1C.”
Shouldn’t that be enough?
Quick teaching moment. The hemoglobin A1C is a measurement that averages blood sugar levels over the past two to three months. Someone whose pancreas is not on permanent vacation typically has an A1C somewhere between the 4% and 5.5% range. Levels between 5.7% and 6.4% indicate prediabetes, while 6.5% or higher indicates diabetes. So yes, it’s a diagnostic tool, and it’s a tool in diabetes management.
In other words, it’s the academic report card of your red blood cells. (We’ll come back to that idea later.)
The A1C doesn’t care if you pre-bolused. It doesn’t care if you walked after dinner to try to get your blood sugar down. And it definitely doesn’t care if you rage-bolused afterward because the walk didn’t work.
Before we jump in, I want to say something clearly: A1C matters. It’s an important clinical marker. It helps guide treatment decisions. It gives us a snapshot of glucose patterns over time. As a clinician, I use it. As a person living with diabetes, I track it.
So yes, it’s important.
But perhaps not in the way that you think. Because somewhere along the way, we turned it into a scoreboard. And diabetes already has enough numbers, doesn’t it?
The A1C Reveal
There’s a segment of the diabetes world that proudly shares their A1C number:
“Mine is 5.7.”
“Mine is 5.2.”
“Mine is 6.”
Your endo might even make a big deal if it’s a “good” number. I understand the impulse. Truly, I do. It’s a way of saying:

“I work hard.”
” I pay attention.”
“I’m doing this well.”
I’ve been there too. In my younger days, I actually made a T-shirt with the Ironman triathlon silhouette and “6.5” printed inside of it.
Nothing says “balanced emotional relationship with a lab value” like screen-printing it onto cotton. I was proud. I wanted to show it off. It felt like proof of effort.
But here’s the truth: The number doesn’t always reflect the work.
A Chemistry Lesson
In college, I took Chemistry. And spoiler alert: I was not a good chemistry student.
The first time I took it (yes, “first” tells you there was a second), I worked really hard, but to no avail. The professor took pity on me and passed me with a D. As a Type A personality, that wrecked me.
So I retook it. Office hours. Flashcards. Study groups. The whole montage. But even studying harder than I ever had, grinding through every equation… I got a C. A C+, but a C nonetheless.
Did I not work hard? No. In fact, I worked my ass off in that class.
It’s funny, but in the first draft of this post, I included the fact that I retook Chemistry when I was applying to nursing school, and in that draft, I included the grade.
Why did I feel the need to include the grade in that first draft? Because many of us, myself included, associate numbers with effort. The number is either “good” or “bad,” and we quietly attach that “good” or “bad” to ourselves. And on first impulse, it was very important to me for you to know that I was now “good.”
Translation: Good grade? I’m smart. Bad grade? I’m not.
Translation for Diabetes: Good A1c? I’m disciplined. Bad A1c? I must not be trying hard enough.
We assume the grade tells the whole story. But it rarely does.
When Numbers Become Identity
Somewhere along the way, we didn’t just make A1c a scoreboard. We made it a character reference. We label the A1c as “good” or “bad.”
A “good” A1c means you’re responsible. In control. Disciplined. A Rock Star.
A “bad” A1c means you slipped. You weren’t careful enough. You do not care
But A1C is not a morality test. It’s biochemistry. And when we attach “good” or “bad” to it, while some of us might be just describing glucose patterns, others (both with and without diabetes) are assigning a value to the person behind the pancreas. That’s where it gets dangerous.
Because if the number is “good,” we feel proud. If it’s “bad,” we feel shame. And shame is a terrible long-term diabetes management strategy. Shame doesn’t improve insulin sensitivity. It doesn’t lower cortisol. It doesn’t make someone more likely to check their glucose tomorrow.
It just makes them feel smaller. And diabetes already takes up enough space.
Now I’m the Dad Saying It
Ironically, as a father, I now find myself on the other side of this type of conversation with my daughter. When she doesn’t doesn’t receive a high grade on a project or test, she beats herself up. And I find myself saying the same thing over and over:
“As long as you worked hard, I don’t care about the grade. That’s what matters to me.”
Not perfection. Not a comparison. Not someone else’s grade.
But instead, effort. Growth. Resilience.
And that’s how it should be with A1c too.
When Dexcom and Abbott created their dashboards, they did something subtle, but amazing: they started reporting the percentage of time the sensor is worn. That’s an enormous win for diabetes self-worth. Because wearing it does indicate effort. It’s actually the first thing I comment on when I’m reviewing data with a patient.
“Look at this, you’re wearing it 90% of the time. That’s fantastic.”
And it is fantastic. Because engagement matters. And it’s a heck of a lot easier to have a constructive conversation about patterns, corrections, and time in range when you acknowledge the effort before you discuss management strategies.
That’s the shift. From moralizing the number to recognizing the work.
A1C Is Important. But It’s Not Your Worth.
Let me be clear: this is not an anti-A1C post. A1c is important. It gives us useful information. It can highlight risk. It can guide change.
But it is not:

A measure of your discipline.
A measure of your intelligence.
A measure of your moral character.
A measure of how much you care.
Two people can work equally hard and have very different A1Cs:
Different bodies.
Different stress levels.
Different hormones.
Different life seasons.
Different access to care.
Different sleep.
Same effort. Different number.
From “6.5” to “I Know My A1C”

I found the shirt I described above in a box of old trophies and triathlon paraphernalia, but I decided I’m not going to wear it again. Maybe I’ll make a new one. Instead of 6.5, it will simply say: “I know my A1C.”
That’s it.
The number? That’s my business, and if I share it, it won’t have anything to do with how I feel about myself. If someone with diabetes tells you they know their A1C, the correct response is:
“That’s great.”
Because knowing it means you’re engaged. It means you’re paying attention. It means you care. And caring is the work.
The number is just the data. And that should be enough.