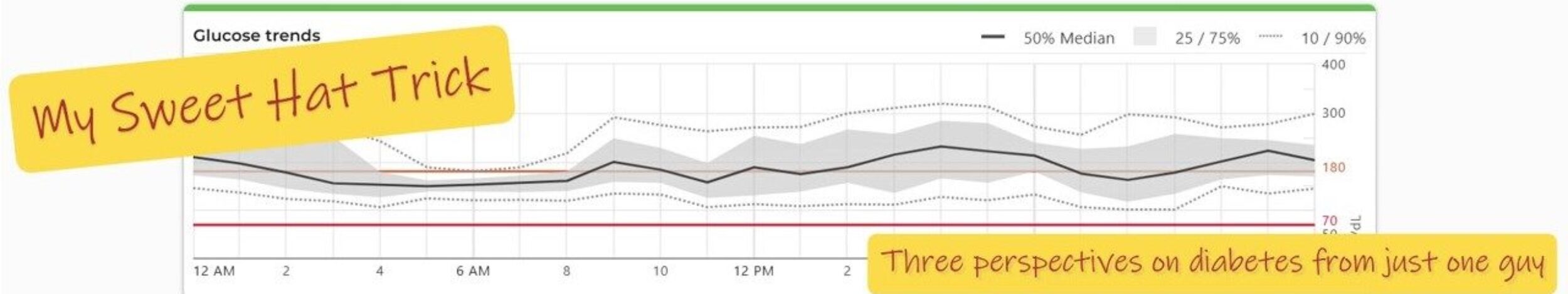
Yesterday was my final prep run for the endurance race I’ve got coming up in a couple of weeks. (No need to share the distance—let’s keep the illusion of balance alive a little longer.)
When the temperature rises, so does the motivation to get outside and get moving. Whether you’re walking, biking, chasing your kids around the backyard, or trying to outrun the dog who stole the freeze pops (my preferred way to treat a low in the summer), exercise during the summer can be energizing—and a little tricky if you live with diabetes.
As someone who lives with diabetes and works in the field, I know firsthand how important it is to stay active while keeping safety in mind. So here’s a guide to getting your sweat on—without your glucose (or your CGM) melting down.
Hydration Is More Than Just a Buzzword

If you have diabetes, you’ve probably heard “Drink water!” so many times that you could use it as your ringtone. But seriously, hydration matters. Dehydration can lead to stubborn blood sugars, sluggish workouts, and that delightful raisin feeling in your mouth.
Pro tip: If you’re sweating buckets, you’ll need to take in electrolytes along with water. Most sports drinks have them. And depending on how you’re managing your blood sugars, you can either go for the low-sugar option or the “Suga, Suga, Suga” kind. Just check the carbs and serving size—many bottles contain more than one serving.
Humidity: The Sticky (and Sneaky) Factor
When I was a teen, I used to run a local 10K on Memorial Day. I could never understand why I didn’t need to eat as much for that race as I did for a 10K that would take place in February. Now I know better: humidity doesn’t just mess with your comfort—it can mess with your blood sugars too.
When your body is under heat stress, cortisol and other stress hormones can rise, which may cause blood sugar to creep up. And if you’re not drinking enough water, dehydration can concentrate glucose in your bloodstream like an extra-strength slushy.
Translation: You might be doing everything right—eating well, moving your body—and still see unexpected highs. Welcome to the frustrating-but-fixable world of summer diabetes.
Here’s how to fight back:
- Hydrate like it’s your job. Because honestly, in summer, it kind of is.
- Consider your patterns. If you consistently see highs after a hot, humid walk, it might be the heat talking.
- Log it. Learn from it. Laugh if you can. Then adjust your plan accordingly.
Humidity also creates a physical problem: nothing wants to stick. Once CGMs and infusion sets start to peel off, they’re nearly impossible to keep in place.



So plan ahead:
- Prep your skin: Use an alcohol wipe, let it dry, then apply like you mean it. Make sure you’re doing changes well before entering sweat mode – an hour is nice, but two or three is better.
- Stick with support: Skin Tac, barrier wipes, or liquid adhesive can work miracles—just don’t get them on your fingers unless you want to glue yourself to the steering wheel.
- Try overlays: GrifGrips, Simpatch, ExpressionMed, and Skin Grips are like adhesive bodyguards; they’ve been designed for every type of infusion set, sensor, and even for Omnipod, and Tandem Mio)
- Use sleeves or bands: Especially helpful for kids, active adults, or anyone who sweats like a faucet during a 10-minute walk.
Humidity might win a few battles, but with the right prep, you’ll win the match.
Insulin and the Summer Heat: Diva Behavior Ahead
Speaking of high blood sugars, insulin is kind of like that one friend who’s amazing—but only if the lighting, temperature, and vibe are just right. Once temps creep past 86°F (30°C), which tends to be pretty common in the summer, your insulin may start to lose its cool—literally. And when insulin gets cranky, it doesn’t work as well. That means more mystery highs and fewer predictable responses, no matter how good your carb-counting game is.
So don’t leave it in the car. Don’t tuck it in your sock. And don’t pretend your black running shorts are a climate-controlled environment.

Instead:
✅ Keep it in the shade like a tired houseplant.
✅ Use an insulated pouch or cooling case (Frio packs: because insulin deserves spa treatment).
✅ If you wear a pump, try to keep it under light, breathable clothing—no sunbathing for your basal rates.
Remember: insulin is a life-saving hormone, but it’s also a bit of a diva. Treat it right, and it won’t ghost you mid-workout.
Time Your Workouts Wisely

If I have to exercise at noon in July, it’s basically self-microwaving. Early mornings and evenings are cooler, quieter, and come with fewer curious neighbors watching you check your CGM mid-squat.
Personal trick: On Wednesdays, I run during my daughter’s soccer practice. She gets to score a goal; I get in my run. Then we both get to soak the car seats on the drive home—family bonding at its finest.
Watch for Low Blood Sugar (and Highs Too!)
Heat can make insulin act faster, which is cool… until it’s not. You might drop quicker than expected, and your body might not be too subtle about it. Or, thanks to dehydration and stress hormones, you could go high. Because diabetes is all about keeping things interesting, right?
Always pack low treatments. Glucose tabs melt? Try fruit pouches, juice boxes, or frozen freeze pops. I’ve even run with honey packets—sticky but effective. (Pro tip: Share with the kids at your own risk.)
Foot Care Still Matters (Yes, Even in Flip-Flops)
Sandy pool decks, mystery grass, and shoes with questionable support—summer is full of foot hazards. If you have neuropathy, inspect your feet daily. If you don’t have neuropathy, inspect your feet daily.
Sandals are fun until they become tetanus auditions.
Also, if you wear socks with sandals, you’re either an absolute genius or my new style icon. No judgment here.
And don’t forget about the insulin
While we’re worrying about water, the sensor staying on and the humidity. don’t forget about the insulin integrity.
You might be doing everything right—eating well, moving your body—and still see unexpected highs.
Dress for (Glucose) Success
Lightweight, breathable clothing helps regulate your body temperature and keeps your tech from sliding off. Hats help too—especially the ones that make you look like a park ranger on vacation.
And if you’re testing new adhesives this summer, now’s a great time to log what works… and what flew off mid-jog and stuck to your neighbor’s mailbox. (Sorry, Steve.)
Make It a Family Affair
Exercise doesn’t have to be structured. It can be chasing your kids, having a water balloon fight, or arguing with your partner (again) about who left the CGM scanner in the car.
In our house, chasing the dog and dodging low alarms basically counts as interval training. And we’re okay with that.
Final Thought
Living with diabetes means always having a plan—and a backup plan. But it also means being creative, resilient, and just a little sweaty.
Summer exercise doesn’t have to be intimidating. With a little preparation and a healthy dose of humor, you can enjoy all the movement the season has to offer.
Let’s make this the summer of sweaty success, stuck-on sensors, and blood sugars that (mostly) cooperate.
There are many other types of products out there that you can use to keep the sensor and sites attached. Feel free to leave your favorites in the comment section.